Ontario Tech researcher asks: Can we be faster at identifying positive COVID-19 cases?
Leading international health informatics expert Dr. Carolyn McGregor concerned about gap between COVID-19 onset and confirmation dates
January 22, 2021
![Dr. Carolyn McGregor (left) consults with members of her research team in 2018 in the Health Informatics Research Laboratory at Ontario Tech University (with Catherine Inibhunu [centre] and Roozbeh Jalali).](images/thumbnail-healthinformatics.jpg)
As Canada nears the one-year anniversary of the first fatality related to COVID-19, the grim data of case numbers continues to paint a challenging picture for health-care experts.
Every day, Ontario and other jurisdictions release new numbers about COVID-19 cases, with a particular focus on the number of confirmed positive tests. However, in most cases there is a ‘lag time’ between case confirmation and the exact date that each patient first experienced the onset of COVID-19 symptoms.
The time discrepancy between COVID-19 onset and the date of reporting is of particular concern for Ontario Tech University researcher Dr. Carolyn McGregor. The Faculty of Business and Information Technology professor has been closely analyzing daily data in Ontario and comparing it with similar case-reporting numbers from the states of Victoria and New South Wales in her native Australia.
“People with COVID-19 are most infectious before the onset of their symptoms,” says Dr. McGregor, Ontario Tech’s Research Excellence Chair in Health Informatics. “So making sure the testing, results, and contact-tracing notification process happens quickly is extremely important. Victoria in Australia has been able to drop cases down rapidly, so I was very interested in uncovering how they’ve accomplished that and what those lessons are.”
Dr. McGregor is the Founding Director of the Joint Research Centre in Artificial Intelligence for Health and Wellness between Ontario Tech University and the University of Technology Sydney. Through reports from family members in Australia about when they’ve had to isolate, she’s also been able to keep tabs on how her home country handles and reports COVID-19 data.
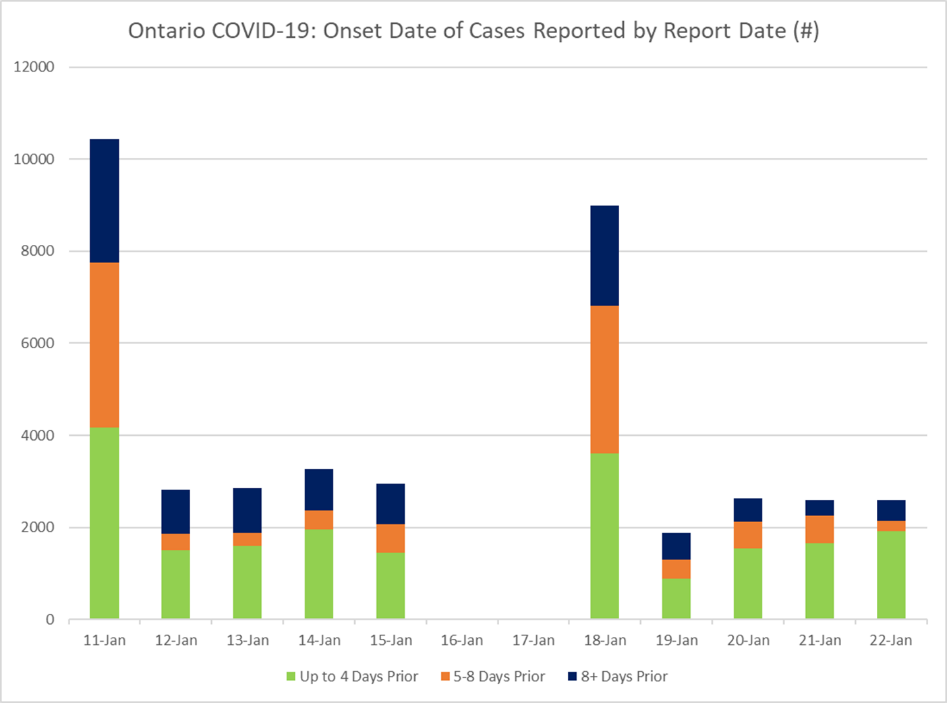
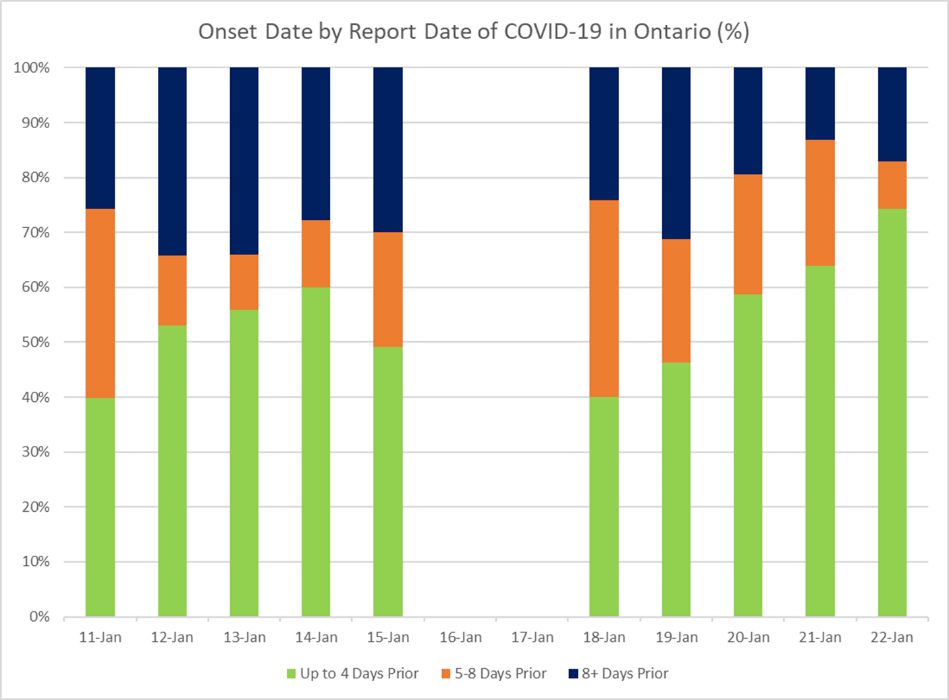
“The real difference between Ontario and Australia at this point is the time it takes to report cases,” says Dr. McGregor. “I noticed that a lot of the cases being reported in Ontario had onset several days earlier than I expected. When I started tracking this on January 11, only 40 per cent of cases reported that day had onset within the previous four days. Many cases, in fact, were at least eight days old (onset on January 3 or earlier).”
If public health is contacting positive cases and doing contact tracing more than four days after the onset of symptoms in hundreds or even thousands of patients, then all of those patients’ contacts have still been circulating for a long time as well. These yet-to-be-announced cases mean those patients who are not yet isolating may also still be infecting others.
“Victoria, Australia was able to crush the number of cases through early case confirmation and receiving military assistance with positive case contact and contact tracing,” she says. “Are Canada’s provincial governments aware that we are this far behind with case onset dates?”
A public inquiry into the Victorian Government’s COVID-19 contact tracing system and testing regime (PDF) concludes the ideal turnaround time for conducting tests and reporting positive cases is ‘within 24 hours’. If a positive case’s close contacts are notified within 48 hours, onward transmission is reduced by up to 40 per cent. Each subsequent one-day delay in reporting results dramatically erodes the potential effectiveness of contact-tracing efforts.
Dr. McGregor says implementing much faster reporting protocols would significantly reduce Ontario’s positive-case replication rates. Taking four days, or more than eight days to report after the onset of a patient’s symptoms will not allow Ontario to replicate Australia’s model of success.
‘It may be a case of having more resources for labs and test processing to be able to catch up and be more current with the data,” she says. “My point is that if we don’t fix the issue of how far behind the testing, results and tracing is, then when we reopen we will have lots of contacts of positive cases not learning early enough that they need to quarantine. This will result in additional subsequent cases that could be avoidable. Sometimes it is the subtle messages in the data that are key. The earlier we are able to identify and isolate positive cases, the better.”
- The upward trend of the green bar indicates a promising trend of faster case reporting during the week of January 18 to 22.
Media contact
Communications and Marketing
Ontario Tech University
communications@ontariotechu.ca